- Pharmacology
- Allergy, Immunology, and ENT
- Cardiology
- Emergency Medicine
- Endocrinology
- Adolescent Medicine
- Gastroenterology
- Infectious Diseases
- Neurology
- OB/GYN
- Practice Improvement
- Gynecology
- Respiratory
- Dermatology
- Mental, Behavioral and Development Health
- Oncology
- Rheumatology
- Sexual Health
- Pain
Teen With Progressive Depigmented Patches
This 16-year-old boy had slowly progressive hypopigmented lesions onthe lower extremities for the past 4 years. He also had atopic dermatitis,asthma, and allergic rhinitis.
HISTORY
This 16-year-old boy had slowly progressive hypopigmented lesions on the lower extremities for the past 4 years. He also had atopic dermatitis, asthma, and allergic rhinitis. His 38-year-old mother had Hashimoto thyroiditis. None of his immediate family members had a similar skin disorder.
PHYSICAL EXAMINATION
Well-demarcated, depigmented patches on extensor aspects of lower legs. Remaining findings unremarkable.
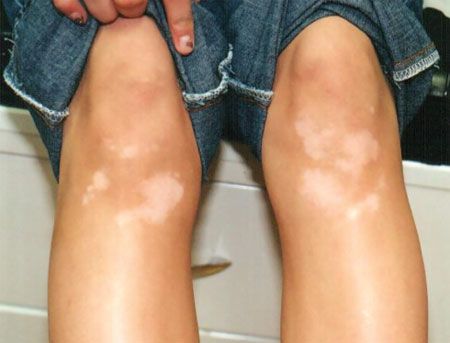
WHAT’S YOUR DIAGNOSIS?
Answer and discussion on next page.
ANSWER: VITILIGO
Vitiligo is a common acquired pigmentation disorder characterized by depigmented macules/patches as a result of loss of functional cutaneous melanocytes.1,2 Because of its unsightly appearance, the condition can have considerable impact both psychologically and socially.3
PREVALENCE Vitiligo is estimated to affect 0.5% to 1% of the population worldwide.4,5 Its onset occurs before age 10 years in about 25% of affected persons, before age 20 years in 50%, and before age 40 years in 95%.6 It is rarely present at birth.3 No differences in rates of occurrence according to race or skin type are apparent, although the condition is more noticeable in dark-skinned persons.5 The sex ratio is about equal.5,7 Vitiligo is more common in atopic patients and in patients with a personal or family history of autoimmune disease.6
ETIOPATHOGENESIS The cause of vitiligo is multifactorial and polygenic. Genetic, immunological, and neurogenic factors may play a role.4,5 It is estimated that 12% to 35% of affected children and adolescents have a family history of vitiligo.8 Inheritance may involve genes associated with regulation of autoimmunity, melanin biosynthesis, response to oxidative stress, and cell adhesion.7,9 For instance, the gene NALP1, encoding NACHT leucine-rich repeat protein 1, predisposes persons to vitiligo and various autoimmune diseases.3,5 Vitiligo is often associated with Hashimoto thyroiditis and Graves disease.7 The involvement of autoimmunity in the pathogenesis of vitiligo (especially in nonsegmental vitiligo) is supported by the demonstration of circulating autoantibodies to melanocytes in affected patients.4,7
Accumulation of free radicals toxic to melanocytes may lead to their destruction.7 Alternatively, melanocytes might exhibit increased sensitivity to oxidative stress.6 Trauma and friction (Koebner phenomenon) may also be involved in the pathogenesis of the disease.2,5,8
In segmental vitiligo, a neurogenic sympathetic disturbance might be responsible.5 Certain chemical mediators released from nerve endings might cause decreased melanin production or destruction of melanocytes.5,7 In this regard, elevated neuropeptide Y levels have been demonstrated in skin of affected persons.7
HISTOPATHOLOGY Histologically, melanocytes are absent in established lesions.2,6 A superficial dermal lymphocytic/mononuclear infiltrate may be seen in the advancing margin of vitiligo, especially in early lesions.2,7
CLINICAL MANIFESTATIONS The amelanotic macules/patches of vitiligo typically appear chalk- or milk-white.7 Lesions often show homogeneous depigmentation and are well demarcated.5 Pinpoint depigmentation may precede patchy depigmentation in rapidly progressing disease.5 A hyperpigmented rim at the interface of depigmented and normally pigmented skin may be seen after sun exposure.5 Lesions are often symmetrical and enlarge centrifugally in size with time.7 The most common locations are the face, followed by the neck, lower limbs, trunk, and upper limbs.6 The back is relatively spared.6 Rarely, the hair, buccal mucosa, and gingiva may also be affected.6
Vitiligo is classified into subtypes on the basis of the pattern and extent of involvement:
• Generalized vitiligo, also known as vitiligo vulgaris, is the most common type and accounts for 33% to 78% of cases.8
Lesions are widely distributed and usually symmetrical,7 as was the case in this patient.
• Universal vitiligo involves more than 80% of the body surface area and is very rare.2
• Focal vitiligo presents as a solitary macule or a few macules in a localized area and in no particular pattern.10
• Segmental vitiligo represents unilateral macules in a dermatomal pattern.10 This type is less likely to be associated with autoimmune diseases.7
Segmental vitiligo is more common in children (accounting for 4% to 19% of cases) than in adults.10
• Acrofacial vitiligo affects periorificial areas and digits.10
• Mucosal vitiligo involves mucous membranes.7
• Trichrome vitiligo has different degrees of depigmentation.10
DIAGNOSIS The diagnosis is mainly clinical, based on the characteristic appearance of the depigmented macules/patches and their propensity to enlarge.2 Wood lamp accentuates the lesion and may be of benefit in the diagnosis, especially in persons with skin type I and type II.11 A skin biopsy is usually not necessary except when the diagnosis is in doubt. A dopa stain for tyrosinase or a Fontana-Masson stain for melanin can be used to confirm the diagnosis.
LABORATORY STUDIES Because of the association with autoimmune diseases, annual screening with a complete blood cell count, thyroid-stimulating hormone, antithyroglobulin antibody, antithyroid peroxidase antibody, fasting blood glucose, and antinuclear antibody is often recommended for children with active vitiligo.6,12
DIFFERENTIAL DIAGNOSIS The differential diagnosis includes pityriasis alba, tinea versicolor, hypomelanosis of Ito, nevus depigmentosus, tuberous sclerosis, nevus anemicus, achromic nevus, oculocutaneous albinism, idiopathic guttate hypomelanosis, lichen sclerosis, piebaldism, and hypopigmentation (postinflammatory, chemical-induced, or drug-induced).2,5,10 The distinctive features of each condition allow a straightforward differentiation from vitiligo.
COMPLICATIONS Affected skin is at risk for sunburn. In addition, vitiligo can be cosmetically and psychologically devastating, resulting in lower self-esteem, poor body image, social anxiety, peer rejection, depression, and stigmatization.3,4 The psychological impact is greater in dark-skinned persons, female patients, and in those with lesions in visible areas.10
Vitiligo is also associated with primary open angle glaucoma.13 The exact mechanism is unknown; however, glaucoma is about 3.5 times more likely to develop in patients with long-standing vitiligo (13 or more years).13
PROGNOSIS The clinical course is generally unpredictable.2 Most patients experience slow progression of the disease through the appearance of new lesions or enlargement of existing lesions.12 There may be periods of relative inactivity, which may last months to years.4 In segmental vitiligo, lesions tend to progress rapidly at onset and show a more stable course thereafter.4 Spontaneous repigmentation of vitiligo is uncommon and is usually incomplete.9,14
MANAGEMENT In children with skin type I and type II, no active treatment other than the use of camouflage cosmetics and sunscreens is usually necessary.11 Tattooing pigment can be used to cover lesions on the lips.15 Psychological support should be offered when necessary.
For patients who prefer treatment for cosmetic reasons, a variety of options are available. The therapeutic effect of all the treatments varies greatly from one patient to another, and treatment must be individualized. Topical corticosteroids and calcineurin inhibitors (tacrolimus and pimecrolimus) are the treatment of choice for those with localized disease.2,10 Potent or very potent topical corticosteroids may arrest the attack on melanocytes by the immune system and can repigment vitiligo.3,11 Topical tacrolimus and pimecrolimus block the action of calcineurin, thereby downgrading the transcription of genes encoding proinflammatory cytokines.13 Topical calcineurin inhibitors are effective in repigmentation of vitiligo; have a better safety profile; and are generally preferred for lesions on the face, neck, genitalia, and intertriginous areas.5,12 Consider narrowband UVB phototherapy for those who have widespread or localized vitiligo associated with a significant impact on quality of life and in those who do not respond to treatment with topical corticosteroids and calcineurin inhibitors.11 Surgical techniques, such as minigrafting, are not recommended for children.16
In several studies, etanercept and infliximab, used for other indications, were found to reduce or halt progression of vitiligo lesions refractory to other treatments.17-19 More research is needed in this area.
References:
REFERENCES:
1.
Leung AK. Vitiligo. In: Leung AK, ed.
Common Problems in AmbulatoryPediatrics.
New York: Nova Science Publishers, Inc. In press.
2.
Lotti T, Gori A, Zanieri F, et al. Vitiligo: new and emerging treatments.
Dermatol Ther.
2008;21:110-117.
3.
Whitton ME, Pinart M, Batchelor J, et al. Intervention for vitiligo.
CochraneDatabase Syst Rev.
2010(1):CD003263.
4.
Matin R. Vitiligo in adults and children.
Clin Evid.
2008;pii:1717.
5.
Taïeb A, Picardo M. Clinical practice. Vitiligo.
N Engl J Med.
2009;360:160-169.
6.
Mazereeuw-Hautier J, Harper J. Vitiligo. In: Harper J, Oranje A, Prose N,eds.
Textbook of Pediatric Dermatology.
Oxford, UK: Blackwell Publishing;2006:1041-1056.
7.
Halder RM, Chappell JL. Vitiligo update.
Semin Cutan Med Surg.
2009;28:86-92.
8.
Huggins RH, Schwartz RA, Janniger CK. Childhood vitiligo.
Cutis.
2007;79:277-280.
9.
Silva de Castro CC, do Nascimento LM, Walker G, et al. Genetic variants ofthe DDR1 gene are associated with vitiligo in two independent Brazilian populationsamples.
J Invest Dermatol.
2010;130:1813-1818.
10.
Isenstein AL, Morrell DS, Burkhart CN. Vitiligo: treatment approach inchildren.
Pediatr Ann.
2009;38:339-344.
11.
Gawkrodger DJ, Ormerod AD, Shaw L, et al; British Association of Dermatologists,Royal College of Physicians of London, Cochrane Skin Group, VitiligoSociety. Guideline for the diagnosis and management of vitiligo.
Br J Dermatol.
2008;159:1051-1076.
12.
Silverberg NB, Travis L. Childhood vitiligo.
Cutis.
2006;77:370-375.
13.
Rogosic V, Bojic L, Puizina-Ivic N, et al. Vitiligo and glaucoma-an associationor a coincidence? A pilot study [published correction appears in
ActaDermatovenerol Croat.
2010;18:119].
Acta Dermatovenerol Croat.
2010;18:21-26.
14.
Lo YH, Cheng GS, Huang CC, et al. Efficacy and safety of topical tacrolimusfor the treatment of face and neck vitiligo.
J Dermatol.
2010;37:125-129.
15.
Singh AK, Karki D. Micropigmentation: tattooing for the treatment of lipvitiligo.
J Plast Reconstr Aesthet Surg.
2010;63:988-991.
16.
Gelmetti C, Frasin A, Restano L. Innovative therapeutics in pediatric dermatology.
Dermatol Clin.
2010;28:619-629.
17.
Rigopoulos D, Gregoriou S, Larios G, et al. Etanercept in the treatment ofvitiligo.
Dermatology.
2007;215:84-85.
18.
Simón J-A, Burgos-Vargas R. Vitiligo improvement in a patient with ankylosingspondylitis treated with infliximab.
Dermatology.
2008;216:234-235.
19.
Campanati A, Giuliodori K, Ganzetti G, et al. A patient with psoriasis andvitiligo treated with etanercept.
Am J Clin Dermatol.
2010;11(suppl 1):46-48.
Recognize & Refer: Hemangiomas in pediatrics
July 17th 2019Contemporary Pediatrics sits down exclusively with Sheila Fallon Friedlander, MD, a professor dermatology and pediatrics, to discuss the one key condition for which she believes community pediatricians should be especially aware-hemangiomas.
Tapinarof cream 1% demonstrates efficacy in atopic dermatitis patients with skin of color
March 8th 2024Data from a pair of identical, phase 3, double-blind, randomized, and vehicle-controlled trials were presented at the 2024 American Academy of Dermatology (AAD) Annual Meeting in San Diego, California.
